GENERAL NEUROLOGY
Pupillary response
Updated on 14/10/2024, published on 11/10/2024
- examination of the pupils helps localize lesions in the visual pathways and autonomic nervous system
- aids in monitoring neurological status (changes in pupil size, shape, and reactivity can indicate brainstem lesion, increased intracranial pressure, or impending herniation) → Pupillary response in unconscious patients
- pupillary responses provide insight into sympathetic and parasympathetic integrity
Anatomy and physiology
Pupillary muscles
- iris sphincter muscle (sphincter pupillae) is composed of smooth muscle fibers arranged in a circular pattern around the pupillary margin of the iris
- it contracts to decrease the pupil’s diameter in bright light or during near vision (accommodation)
- it is under parasympathetic control
- iris dilator muscle (dilator pupillae) is radial in orientation
- it dilates the pupil (mydriasis) in response to low light conditions, stress, or as the “fight-or-flight” response
- it is under sympathetic control
Centers and pathways
Parasympathetic pathway (pupillary constriction – miosis)
- Edinger-Westphal nucleus (midbrain) → preganglionic fibers travel with the oculomotor nerve (CN III) → ciliary ganglion → postganglionic fibers innervate the sphincter pupillae muscle (via short ciliary nerves)
- constricts the pupil in response to light and during accommodation
- neurotransmitter: acetylcholine
- receptors: muscarinic cholinergic receptors (primarily M3 subtype)
Sympathetic pathway (pupillary dilation – mydriasis)
- hypothalamus → ciliospinal center of Budge (spinal cord levels C8–T2) → preganglionic fibers exit the spinal cord and ascend to the superior cervical ganglion → postganglionic fibers travel along the internal carotid artery, through the cavernous sinus, and reach the dilator pupillae muscle (via the long ciliary nerves)
- dilates the pupil in response to darkness (to increase light entry), stress, or fear
- neurotransmitter: norepinephrine
- receptors: alpha-1 adrenergic receptors
Sudomotor sympathetic pathway
- postganglionic sudomotor fibers are part of the periarterial carotid plexus
- sudomotor fibers for the medial forehead run along the ICA through the carotid canal
- sudomotor fibers for the maxillary and mandibular regions run along the ECA
- preganglionic lesions affect the entire ipsilateral side of the face; manifestation of postganglionic lesions depends on whether the plexus around the ICA or ECA is involved.
Pupillary reflexes
Light reflex
- photoreceptors in the retina → optic nerve (CN II) → pretectal nuclei in the midbrain → bilateral Edinger-Westphal nuclei → sphincter pupillae
- as a result, both pupils constrict when light is shone in one eye (direct and consensual responses)
Near reflex
- pathway involves input from the visual cortex to the Edinger-Westphal nucleus and the oculomotor nucleus (CN III)
- adjusts the optical system for near vision
- pupil constriction improves the depth of focus
- ciliary muscles adjust the lens curvature (accommodation)
- medial rectus muscles turn the eyes inward (convergence)
Clinical examination
- pupil size and shape
- light reflex
- the pupil constricts to direct illumination (direct response) and the illumination of the fellow eye (consensual response)
- both pupils dilate in the dark
- swinging flashlight test →Relative Afferent Pupillary Defect (RAPD) or Marcus Gunn pupil
- near/accommodation reflex
- test requires voluntary effort
- pupillary constriction and eye convergence occur when the patient focuses on a near object (along with accommodation)
Most common abnormalities
- features:
- mydriasis, unreactive to light
- ptosis (due to levator palpebrae superioris paralysis)
- ophthalmoplegia – eye positioned “down and out” due to unopposed lateral rectus and superior oblique muscles
- causes: lesions affecting the oculomotor nerve, such as aneurysms (posterior communicating artery), tumors, or increased intracranial pressure
- features:
- miosis (due to unopposed parasympathetic activity)
- semiptosis – paralysis of the superior tarsal muscle (Müller’s muscle)
- enophthalmos
- anhidrosis on the affected side
- sudomotor fibers for the maxillary and mandibular regions run along the ECA
- sudomotor fibers for the medial forehead run along the ICA through the carotid canal
- disruption of the sympathetic pathway at any point from the hypothalamus to the eye
- first-order neuron lesion (hypothalamus) – stroke, tumor
- second-order neuron lesion (preganglionic) – Pancoast tumor, cervical trauma or surgery, aortic aneurysm
- third-order neuron lesion (postganglionic) – carotid dissection, cluster headaches, cavernous sinus pathology
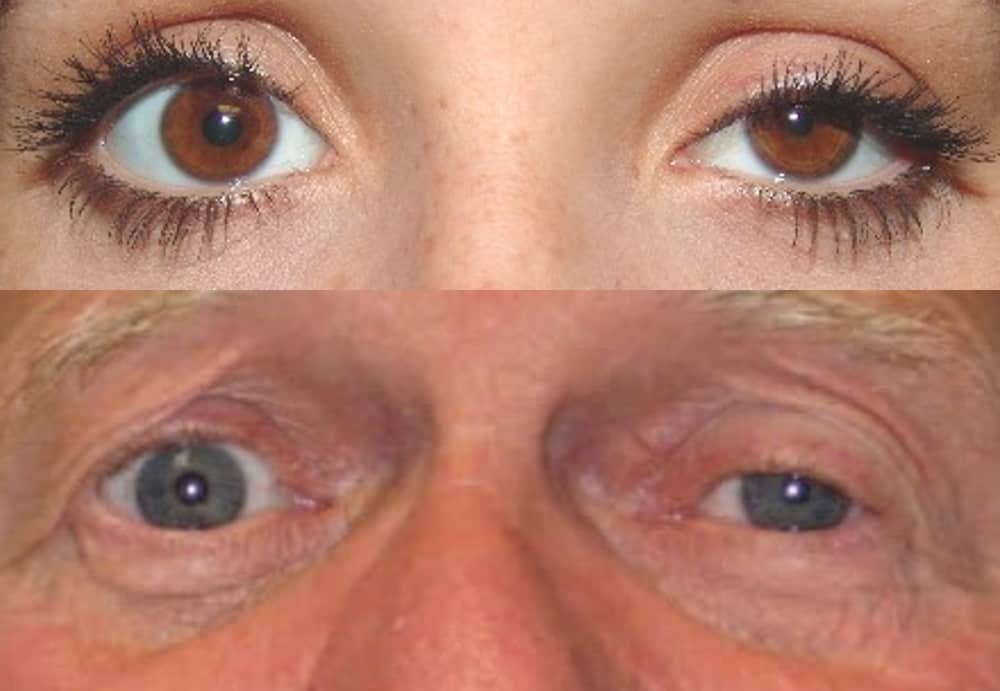
- Adie tonic pupil, also known as Holmes-Adie syndrome, is a neurological disorder characterized by:
- anisocoria with a dilated tonic pupil
- most cases are unilateral (80%) but can become bilateral
- anisocoria is greater in the light compared to in the dark (due to dysfunction of the parasympathetically innervated iris sphincter muscle ⇒ the large pupil is abnormal)
- the pupils constrict more to accommodation than to light
- a slit lamp examination often shows sectoral palsy of the iris sphincter, with vermiform movements of the pupillary margin
- low-dose pilocarpine constricts the tonic pupil more than the normal pupil (due to hypersensitivity of denervated fibers), followed by a slow and sustained relaxation
- loss of deep tendon reflexes (most commonly the Achilles reflex)
- anisocoria with a dilated tonic pupil
- more common in young women
- symptoms: photophobia and difficulty adapting to the dark
- etiology: damage to postganglionic parasympathetic fibers in the ciliary ganglion, often idiopathic, viral, posttraumatic, etc.
- pathophysiology:
- damage to the ciliary ganglion causes denervation hypersensitivity with postsynaptic receptor upregulation
- reinnervation process is often aberrant, and fibers intended for the ciliary body may end up in the pupil (aberrant regeneration)
- as a result, near accommodation produces more miosis compared to the response to light; the reaction is tonic
- affected pupil constricts less (appears to dilate) when the light is swung from the normal eye to the affected eye
- caused by optic nerve damage (e.g., optic neuritis) or severe retinal disease
- small, irregular pupils
- light-near dissociation – pupils constrict poorly to light but normally constrict during accommodation
- classically associated with neurosyphilis (DDx – dorsal midbrain lesion, diabetic neuropathy)